The Quick and Dirty Guide to Pediatric Assessment
Category: Special Populations
Topic: Pediatrics
Level: EMR
Next Unit: Pediatric SVT vs Sinus Tachycardia
41 minute read
The Quick and Dirty Guide to Pediatric Assessment

Although children account for only a small percentage of pre-hospital emergencies, they present a special challenge to EMS professionals; both patient and crew suffer extreme emotional stress and anxiety, in many cases. They aren't “mini-adults”, so their anatomy and physiology including airway, breathing, circulation, muscle, and skeleton system deserve special consideration, since they grossly differ from an adult. The internal organs are in closer proximity and more tightly encased to each other in children than in adults, and this places children at higher risk of traumatic injury due to the "tight quarters". The reaction to pain/illness and the capabilities to deal with it, in children is different depending on their developmental stages.
Developmental Stages
- Infants: 1-12 months - Between 4-6 months most infants have doubled their birth weight; tripling it by the 12 months. In the first year, infants can usually walk and their heart doubles in size, the heart rate slows, and BP starts to increase. Common illnesses will typically affect the respiratory, GI, and CNS, manifesting as:
- Respiratory distress
- Nausea
- Vomiting
- Dehydration
- Seizures
- Meningitis
- SIDS - Toddlers: 1-3 years - Muscle Mass and bone density increases during the toddler stage, normally gaining 2 kg (5 lbs) each year. By age 2 the nervous system is fully developed and functioning. Most are able to control voluntary control of urinary/bowel movements. Basic language skills normally develop by age 3. They begin to notice the difference in male and female. The common illnesses that affect toddlers:
- Respiratory distress
- Asthma
- Bronchiolitis
- Croup
- Nausea
- Vomiting
- Diarrhea
- Dehydration
- Febrile seizure
- Sepsis
- Meningitis - Pre-school age: 4-5 years - During the preschool years, children experience advances in gross and fine motor skills. Illnesses are similar to the conditions mentioned for 1-3 year old but, this age group is more likely to get into trouble. This trouble includes falls, burns, lacerations, and accidental poisonings. Preschoolers are curious and have an urge to explore, but they have no concept of danger until it is too late.
- School age: 6-12 years - The growth of school-aged children is slower and more steady than seen with preschoolers. Most children at this age gain over 3 lbs. and grows 2.5 inches per year. Most illnesses are viral and injuries are more common because of their increased independence and activity.
- Adolescent: 13-18 years - During adolescence, the final stage of change in growth and development occurs. Organs rapidly increase in size and blood chemistry is similar to an adult.
Anatomy and Physiology Review
Head
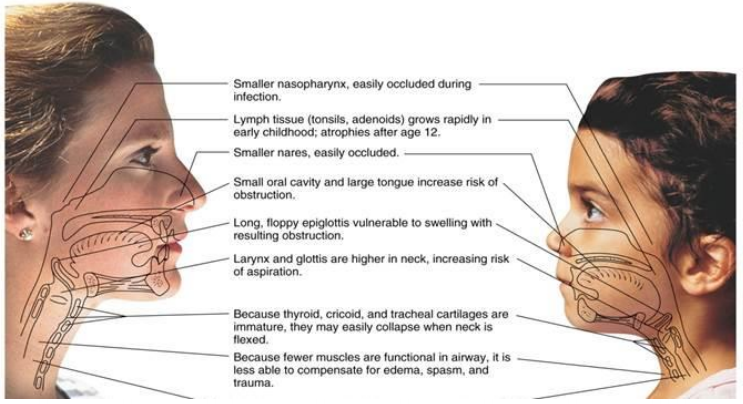
The biggest thing to keep in mind when treating a child is that the differences in infants and children set them apart from the adult patient so, often a review of the anatomy is recommended. A child's head is proportionately larger than adults, accounting for 25% of the total body weight, in newborns especially. Children have a larger occipital region and a face that is smaller compared with the total size of the head. Because of this relative size difference, a high percentage of trauma in children involves the head and face.
When using spinal immobilization for a child <3 years old, it may be indicated to place a small padding under the patient's shoulders to maintain a natural, neutral alignment. A folded sheet placed under the occiput of a severely ill child >3 years old or under the shoulders if the child is <3 years old, can help to establish a sniffing position needed to maintain an adequate airway.
To accommodate for the normal growth of the brain of an infant, the anterior fontanelle remains open and vulnerable to injury for 9 to 18 months after birth. The anterior fontanelle is usually level or slightly below the surface of the skull. A bulging or tight fontanelle indicates possible increased ICP. A sunken fontanelle that is sunken, it suggests dehydration in the infant. EMS professionals should assess the anterior fontanelle in infants and young children who are ill or injured. This is best assessed in an upright sitting position when the child is calm and not crying.
Airway
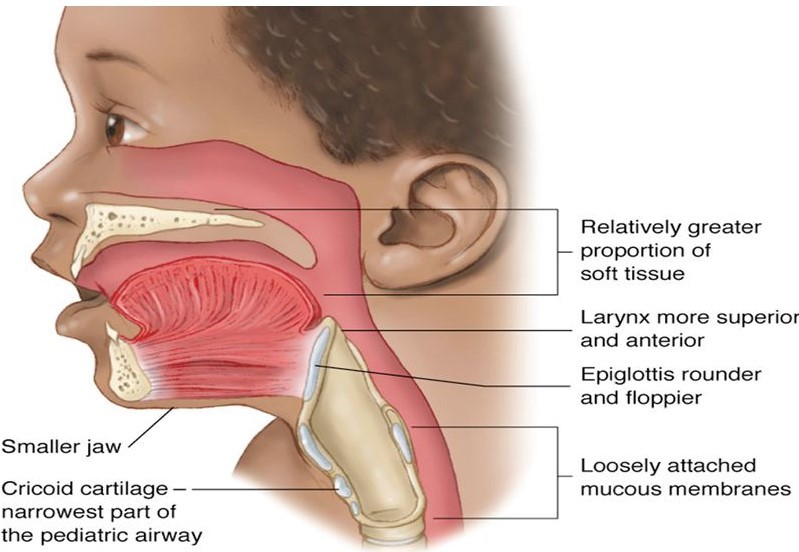
The airway structures of children are narrower and way less stable than an adult's. This naturally makes the airway more vulnerable to obstruction from secretions, obstruction, or inflammation. In addition, the larynx is higher (at the level of C3-C4), more anterior, extending into the pharynx. The tracheal cartilage is smaller in length/diameter and is bifurcated at a higher level than in adults. The cricoid cartilage is the narrowest part of a young child's airway. Proportionately the jaw is smaller and the tongue is larger, increasing the likelihood of an obstruction by the tongue in an unconscious child. The epiglottis is omega-shaped and extends into the airway at a 45* angle. The epiglottic folds are softer and become "floppy", also causing obstruction. Avoid hyperflexion or hyperextension of the patient's neck to avoid airway occlusion. It may be indicated to modify tracheal intubation techniques to ensure a gentle touch on the soft tissues of the trachea, which is very easily injured. Using a straight blade that lifts the epiglottis, choosing an appropriate sized ET tube, and constantly monitor the airway for proper tube placement.
Note: Infants for the first month or so of life are mainly nose breathers. Mucus and secretions in the nares may be enough to cause significant obstruction.
Chest and Lungs
In infants and young children, the chief support for the chest wall comes from immature muscles that are easily fatigued, rather than bones. The use of these muscles for breathing also requires a higher metabolic and O2 consumption rate than older children and adults, causing a build-up of lactic acid in the child's blood. The ribs of a child are more pliable and are positioned horizontally, and the mediastinum is more mobile, offering less chest wall protection to the internal organs within the chest cavity. The lung tissue of children is very fragile, because of this and the limited protection offered by the developing rib cage, pulmonary contusions from trauma and pneumothorax from barotrauma are common in this age group. The thin chest wall allows for easily auscultated breath sounds, which makes assessing adequate breath sounds and confirming ET tube placement difficult in the field. It is a good idea to assess the axillary regions as well as, the anterior and posterior locations in these patients.
Note: When evaluating a pediatric patient who sustained serious trauma, it is important to remember that infants and children are diaphragmatic breathers, which means gastric distention is common.
Abdomen
Like the chest wall, the immature muscles of the abdominal region offer little protection to the already tightly encased organs within the abdomen. The liver and spleen are proportionately larger and more vascular than in adults. This leads to the possibility of multiple organs being injured in the event of significant abdominal trauma.
Extremities
Bones in children are softer and more porous until they reach adolescence. As long bones mature, hormones act on the cartilage, replacing the (softer) cartilage with (harder) bone. The epiphyseal plate (growth plate) lengthens as the bones develop, becoming thicker as new layers are added over old layers. Because of the potential for fracture any sprains, strains, and bone contusions should be treated as if it were a complete fracture. They should be managed with full extremity immobilization and PMS reassessment often. In addition, paramedics must use extreme caution when inserting an IO needle. Improper insertion can cause growth problems for the child for years to come.
Skin
The skin of children is thinner yet more elastic than adults and has less SQ fat. A child has a larger body surface area to body mass ratio. These factors should be considered when an injury occurs or environmental factors are present (Cold-hypothermia, Hot-Hyperthermia, Sun-Sunburn).
Respiratory System
The tidal volume of infants and young children is much less than that of adolescents and adults, but the metabolic requirements for normal breathing are about double, with a smaller residual capacity. Because of these factors, hypoxia can and will rapidly develop.
Cardiovascular System
Cardiac output is rate-dependent in infants and young children, meaning the faster the heart rate, the greater the cardiac output. These patients are not able to increase contractility or stroke volume. The circulating blood volume is proportionately larger than that of adults, yet the overall absolute blood volume is less. The ability to vasoconstrict the vessels helps maintain a viable BP much longer than in adults. Hypotension is a very late sign of shock in a pediatric patient. Therefore, the assessment of shock must be based on the clinical signs of adequate tissue perfusion (i.e., LOC, skin color, cap refill). However, early intervention is required to prevent irreversible or decompensated shock. Special consideration includes:
- The pediatric cardiovascular reserve is vigorous but, limited
- The loss of a small amount of blood/fluid can cause shock
- A child may hide the signs of shock and may be in shock with normal vitals
- Bradycardia is often caused by hypoxia
Note: EMS personnel should suspect shock in any ill/injured child that has tachycardia and evidence of decreased tissue perfusion.
Nervous System
The neural tissue is fragile; nervous system develops throughout childhood. In addition, the anterior and posterior fontanelles remain open for a period of time. Therefore, head injuries involving TBI can be devastating to the infant or young child. The child does have the advantage of superior brain and spinal cord protection from the spinal column and skull.
Metabolic Differences
The way in which children and adults expend energy is different in many ways. For example, infants/children have limited glycogen and glucose stored. Their blood glucose levels can drop dramatically in response to illness/injury, with or without a history of diabetes mellitus. Pediatric patients can lose a significant amount of fluid from vomiting and diarrhea, making them very prone to dehydration. Because of the increased skin surface area, the pediatric patient is susceptible to hypothermia/hyperthermia. For all these reasons, it is important to assess the blood sugar levels and prevent hypothermia by keeping them warm in all ill/injured children.
General Pediatric Assessment
The initial assessment of a child should include looking at the patient and involving the parents in the process. This helps keep them calm and makes the patient more comfortable with the assessment. The parent can offer valuable information that may become vital in the child's treatment. Parents are also the best way to assess the normal mannerisms of the child.
Initial Assessment
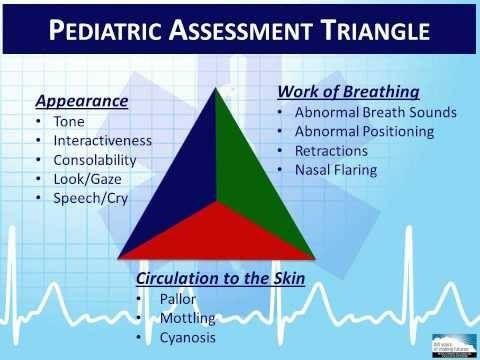
The initial assessment begins with the EMS professional forming a general impression of the patient. The assessment should focus on the details most valuable to the situation, to determine whether a life threat exists. The pediatric assessment triangle is a paradigm that can be used to quickly assess a child (as well as adults, but thats another story for another day) and the potential for immediate interventions. The triangle has 3 components:
- Appearance of mental status and muscle tone
- Work of breathing including rate and effort
- Circulation: assessing skin color/condition
Note: If the child's condition is urgent, focus on the basics (Circulation, Airway, Breathing), stabilization and transporting rapidly but, safely!
Vital Function
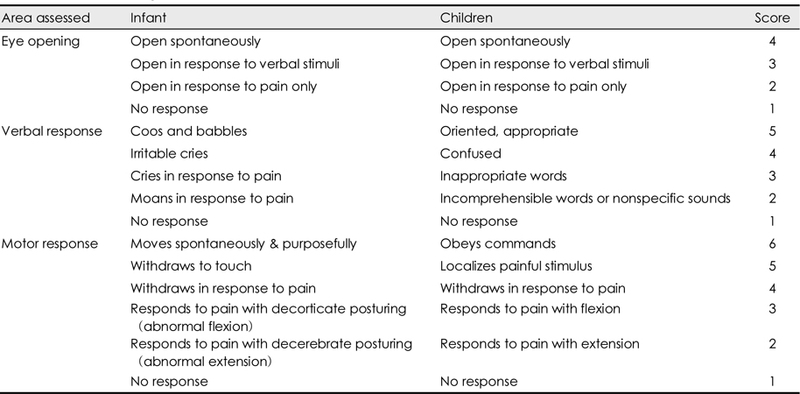
The AVPU scale which assesses, alertness, patients response to verbal stimuli, painful stimuli, or unresponsive or the modified Glasgow coma scale. For details on the pediatric Glasgow coma scale check out Glasgow Coma Scale Made Easy!
Airway & Breathing
The child's airway must be patent, and breathing should proceed with adequate chest wall rise and fall. Signs and Symptoms of respiratory distress include the following:
- Abnormal/absent breath sounds
- Bradypnea/Tachypnea
- Grunting
- Head bobbing
- Irregular patterns to respiration
- Nasal flaring
- Accessory muscle usage
Circulation
Assess the pediatric circulation by comparing the strength and quality of central and peripheral pulses, measuring BP (mainly pts >3), evaluating skin color, temperature, cap. refill, and skin turgor. Assess for the presence of life-threatening hemorrhage and control it.
Focused History
The transition phase is used to allow the child to become more familiar with the crew and equipment, by having conversations and allowing them to touch and play with things that won't hurt them; i.e., a stethoscope. This is only appropriate if the patient is conscious, alert, and not critical. If the patient is critical or unconscious, all interventions should be accomplished while providing a rapid, safe transport to an appropriate facility.
Obtaining a history on an infant, toddler, or preschooler, is nearly impossible. The EMT must obtain reliable information from the caregiver/parent. School-aged adolescents can answer and provide most of the needed information by themselves. The focused history on a pediatric patient can be obtained by using age-appropriate parts of the SAMPLE and OPQRST methods. Important elements of the focused history include:
Chief Complaint
- Nature of illness/injury
- Length of the illness/injury
- Last Meal
- Fever
- Behavior changes
- Vomiting/diarrhea
- Urinary frequency
Medication/Allergies
- Prescribed/OTC medications in the past week
- Any known drug allergies
Medical History
- Any hospital stays
- Physician care
- Chronic illness
Detailed Physical Exam
The physical exam in children should start from head to toe in older children. But, the exam should proceed from toe to head in younger children, normally < 2 yrs old. Depending on the child's condition, the following assessment may be appropriate:
- Pupils: Check for round and reactivity to light
- Capillary refill: Most accurate in children under 6 years old (<2 seconds is normal)
- Hydration: Skin turgor >3 seconds to return, tears present, sunken fontanelle indicates dehydration
Note: When assessing a child who is ill, it is important to note the presence or absence of fever, nausea, vomiting, diarrhea, and urinary frequency.
If time allows and the patient's condition is potentially serious, monitoring of the patient's vitals can provide valuable information. Examples include:
- Blood oxygen saturation (SpO2)
- BP assessment (>3 years old unless medical command requests it)
- Body temperature
- ECG (critical ill/injured)
Ongoing Assessment
The ongoing assessment should be considered appropriate for all patients, but especially pediatrics, and is performed throughout the patient transport. The purpose is to monitor the patient for changes in:
- Respiratory effort
- Skin temp/color
- Mental status
- Vital signs.
There are a number of pediatric resources and aids on the market that break down most of the common medications and pediatric treatments. The Broselow Tape is the most commonly used system used to calculate drug and fluid dosages.

Patient condition, including vitals, should be assessed every 15 minutes in a stable child and every 5 minutes if the patient is critically ill/injured. EMS professionals must be capable of identifying any and all immediate or potential life threats in a child. Obtaining a reliable history and physical exam on a pediatric patient can be challenging at best, and communication tactics are certainly important to their success. There are several AHA certification programs for the proper treatment of pediatric patients, including PALS, PTLS, and many others. They will help to keep you sharp and ready to face the various challenges of managing any pediatric patient.