Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Renal System: Water Balance Response and Buffering
Normal Kidney Function
The kidney:
- Maintains the extracellular environment that is required for adequate functioning of the cells by excreting waste products from metabolism (e.g., urea, creatinine, and uric acid) and by adjusting the excretion of water and electrolytes to match net intake and endogenous production.
The kidney is able to regulate individually the excretion of water and solutes such as sodium, potassium, and hydrogen, largely by changes in tubular reabsorption or secretion.
- Secretes hormones that participate in the regulation of
- systemic and renal hemodynamics (renin, prostaglandins, and bradykinin),
- red blood cell production (erythropoietin), and
- calcium, phosphorus, and bone metabolism (1,25-dihydroxyvitamin D3/calcitriol).
Water's Journey from Intake to Output
The kidneys have specific locations where certain actions take place.
1) Water is taken in by the mouth and goes to the stomach by way of the esophagus. From the stomach, water enters the duodenum and travels through the small intestine and into the large intestine, where much of it is absorbed through the intestinal wall through an osmotic gradient.
In this way, the large intestine is an important part of water balance in the body.
2) Once absorbed, water moves into the intracellular space and then...
3) Flows into the blood vessels in the area and travels around the body as part of the bloodstream, reaching the kidney by way of normal circulation:
First, the water in the blood travels return to the venous system to the liver, then to the heart, then to the lungs, then back to the heart, then through the aorta and down into the kidneys.
H20 → liver → right side of the heart → lungs → left side of heart → aorta → renal arteries → nephrons.
4) In the kidneys,
- blood enters the nephron for filtering, then
- travels to the medullary interstitium and
- then descending loop of Henle where water is reabsorbed. At this location the water in the blood
- enters the principal cells in the collecting duct that move aquaporins to the membrane, allowing water to
- leave the normally impermeable membrane and
- be reabsorbed by way of the vasa recta, which are straight arterioles in the kidney's medullary interstitium.
Water that is not reabsorbed joins the filtered waste products pulled out of the blood and together become urine.
DEFINITIONS:
- Nephron: principle filtering unit of the kidney, made up of Aquaporins--also called water channels, are membrane proteins that form pores in the membrane of biological cells, facilitating water transport.
- Medullary interstitium: internal tissue of the kidney which produces urine.
- Calyces: where urine begins collecting, merging into major calyces, and finally into the renal pelvis (→ ureters → bladder → urethra → urination).
- Renal pelvis: final collection area that is continuous with the ureter.
Urine --> minor calyces --> major calyces --> renal pelvis --> ureter --> bladder.
Urine is moved down the ureters via a peristalsis and collects in the urinary bladder to be excreted either voluntarily or involuntarily by the bladder.
Water Balance
Water is distributed through the intracellular and extracellular fluids of the body.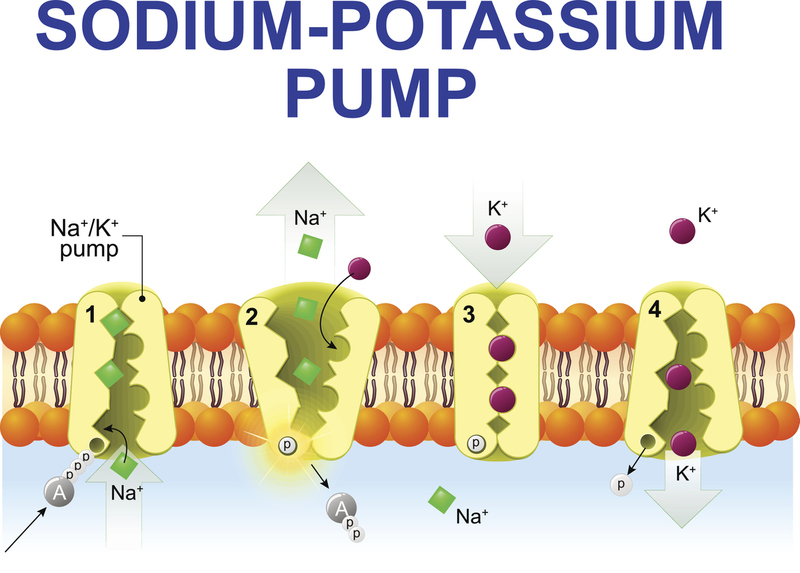
- 2/3 of the water in the body is in the intracellular fluid.
Potassium (K+) and phosphate (PO3−4) are the main ions in intracellular fluid.
- 1/3 of the water in the body is in the extracellular fluid.
The extracellular fluid houses mainly sodium chloride ions (Na+).
The K+ intracellular and Na+ balance is essential for many actions within the body.
Basic concepts involved in the control of fluid and electrolyte regulation include the body's monitoring of extracellular fluid by regulatory mechanisms that sense plasma volume and osmotic concentrations.
WATER FOLLOWS SODIUM: Water moves passively and follows sodium ions, meaning if the sodium concentration increases in either the intracellular fluid or the extracellular fluid, water will also enter that portion of the fluid compartment.
The body will excrete additional electrolytes including sodium in an attempt to equalize the balance between the intracellular and extracellular fluids, thus keeping the sodium and potassium concentrations what they need to be. Similarly, the kidneys can reduce output to increase water uptake to maintain the balance, as well.
Renal Buffering
The buffering system that balances the pH of the intracellular and extracellular fluids include the carbonic acid-bicarbonate buffer system that includes the kidneys, although it does not buffer changes in pH caused by CO2.
The kidneys create bicarbonate in the tubular cells of the distal convoluted tubule and it is here that bicarbonate can be secreted and protons of hydrogen can be absorbed, or bicarbonate can be absorbed and protons of hydrogen can be secreted to maintain a balanced pH. The excess wastes are excreted at the lungs in the form of CO2.
This system is important in compensation for metabolic acidosis or alkalosis.
In the Field
In the field, the EMS responder's main concern is systemic illness that will interfere with the normal kidney functions. This will usually be oliguria as a result of hypovolemia/shock, but you won't be determining if there is oliguria instead, you will be determining whether there IS hypovolemia/shock and if so, all management decisions in such cases rely on
- rapid transport,
- volume repletion,
- maintenance of ABC (airway, breathing, circulation), and
- other supportive measures en route.