Quick and Dirty Guide to Childbirth II: The Delivery
Quick and Dirty Guide to Childbirth II: The Delivery
Delivery

Your main objective when evaluating a pregnant patient is to determine if her complaints are related to active labor and if delivery is imminent. The critical steps to prepare for delivery are:
- Don Proper BSI and prepare any obstetric supplies
- Examine the vagina for crowning
- Feel for uterine contractions in the abdomen
- Take baseline maternal and fetal vital signs
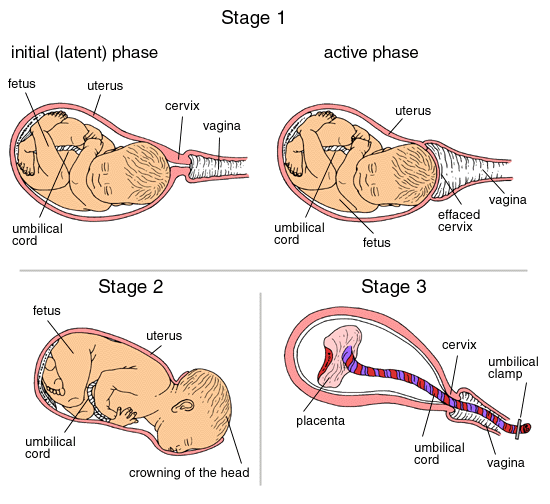
The Stages of Labor/Delivery
Stage I: (Dilation) Regular contractions, thinning and gradual dilation of the cervix, ends with fully dilated cervix (10 cm); Lasts: 12-16 hrs. primipara, 5-7 hrs. multipara
Stage II: (Expulsion) Fully dilated; The time from when the baby enters the birth canal until he is born. This stage lasts 80 min. primipara, 30 min. multipara
Stage III: (Placenta delivery) The time between birth and afterbirth; average time 5 to 30 min.
"Bloody show" begins with the loss of the mucus plug and continues throughout the delivery.
While assessing the patient for signs and symptoms of labor, be sure to ask the right questions:
1. Get her full name and age, for the receiving facility
2. What is her expected due date?
3. Is this her first pregnancy?
4. Has she had prenatal care during the pregnancy?
5. When did labor pains start?
6. Has there been a rush of water or is there any"bloody show" present?
7. Does the patient feel the urge to push?
8. Does the patient feel the need to have a bowel movement?
Never allow a patient you feel may be in active labor to use the toilet
During labor, the mother will experience contractions of the uterus that help the patient's cervix dilate and push the fetus out of the uterus into the birth canal. The contractions will occur at regular intervals, ranging from 30 minutes initially to 1 minute, as imminent labor approaches. Contractions or labor pains last between 30 seconds to 1 minute; if the pain is continuous or prolonged, consider other causes of OB pain.
If the signs and symptoms lead you to believe the patient may be in active labor
Expose the abdomen and genital area while being discrete, professional, and calm. Contractions occurring within 2 minutes of each other should alert the EMT that delivery is imminent. There is no set amount of time that the last stage of labor will last. Every patient is different, especially patients who have had previous childbirths; be prepared for anything! Keep in mind that a first-time delivery usually lasts several hours. Mothers who have previously given birth often know when they are ready to deliver. Labor tends to be shorter after the patient's first child.
Consider transporting the mother if delivery does not occur within 20 minutes of experiencing contractions that are 2-3 minutes apart. Visually inspect for crowning, bleeding, or other signs of an emergency condition that may be causing the patient's symptoms.
When evaluating the mother, keep in mind the four signs of imminent delivery:
- Crowning
- Contractions < 2 minutes
- Rectal Fullness (c/o needing to have a bowel movement)
- A feeling of having to push
Once you have determined that a field delivery is imminent, you should prepare as follows:
- Request a paramedic unit
- Don sterile gloves, gown, and eye protection
- Position mother on her back, with legs up in a partial squatting position
- Provide supplemental oxygen
- Prepare any available OB equipment
- Prepare infant BVM
Presentations that are not able to be successfully delivered in the field:
Note: * Covered in Quick and Dirty Guide to OB Emergencies
- A single limb presentation*
- Prolapsed umbilical cord*
Presentations that can successfully be delivered in the field:
- Normal Cephalic delivery (head first)
- Umbilical cord around the fetus's neck *
- Shoulder Dystocia *
- Butt first *
- Double footling *
Findings Indicating Possible Need for Newborn Resuscitation:
- The patient has received no prior prenatal care
- A Premature delivery
- Labor induced by trauma
- Multiple births
- History of pregnancy problems (i.e., placenta previa and breech presentation)
- Labor induced by illegal drug use (especially narcotics) and alcohol
- Meconium staining when the patient's amniotic sac ruptures (water breaks)
Meconium is the newborn's first stool, it usually occurs well after birth. In some cases, when the pregnancy has gone past full term or the fetus becomes distressed during delivery, the fetus defecates and causes the meconium to mix with the amniotic fluid. If meconium staining is apparent in the fluid or noted on the newborn's face/body, then immediate suctioning and airway control are crucial in preventing serious respiratory problems for the newborn.
OB and Neonatal Care Lecture
Assisting With Delivery
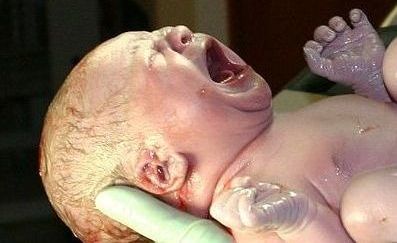
When assisting the mother in delivering her baby, it is important to remember that childbirth is a natural event. In most cases we are just there to "catch".
If the patient has begun the first stage of active labor, the amniotic sac has usually ruptured, expelling the clear amniotic fluid that has protected the developing fetus throughout the pregnancy. The amniotic sac does not always rupture initially, the EMT can pierce it with a gloved hand when the head presents from the birth canal. Make sure to remove the sac from the newborn's nose and mouth because, for the first time, the baby will need them clear in order to breathe.
Delivery Instructions
1. Encourage the mother to breathe deeply between contractions and to push with contractions.
2. As the baby's head crowns, support it with gentle pressure over the perineum and gently support the head during delivery to avoid an explosive birth and prevent injury.
3. If the amniotic sac is still intact, rupture it with a finger to allow amniotic fluid to leak out.
- Note the color and character of the amniotic fluid:
- Normal fluid is clear or straw-colored; Meconium in the fluid produces a pea soup-like color.
4. Suction the mouth and nostrils as needed with a bulb syringe. Squeeze air from the syringe before inserting. Insert the syringe no more than one inch into the mouth and no more than ½ inch into each nostril.
- If you see signs of meconium staining, do not stimulate the infant before suctioning the mouth and nose. This is to avoid aspiration of fecal material that can cause pneumonia.
5. If the umbilical cord is wrapped around the baby's neck, gently slip it over the head DO NOT FORCE IT! If the cord is too tight to slip over the head, apply umbilical cord clamps and cut the cord.
- Clamp and cut the umbilical cord only if the baby's head has emerged and is in a position that allows you to manage the airway. If you are able to free the cord from around the baby's head, hold off clamping until after the baby has been delivered.
6. Encourage the mother to push. Support the baby's head as it delivers.
Caution: babies are slippery!
7. Let the baby come at its own rate; the only intervention that may be required is to gently pull the baby's shoulders down (one at a time) so that it can squeeze through the vaginal opening; however, this shouldn't be required during normal birth. To assist in the delivery of the anterior shoulder, apply gentle downward pressure on the shoulder while continually supporting the newborn's head.
8. As soon as the anterior shoulder has been delivered, apply gentle upward pressure to assist in the delivery of the posterior shoulder.
9. Once both shoulders have been delivered, be ready for the remainder of the body to deliver quickly. Newborn babies are slippery, so handle them carefully.
10. Stimulate the newborn to breathe by tapping the feet, if necessary.
11. Once pulsations have stopped, clamp the cord by placing a clamp approximately 8-10 inches from the baby. Place a second clamp approximately 2 inches from the first, then cut the cord between the clamps. Do not cut or clamp a cord that is still pulsating. Apply one clamp or tie about 10 inches from the baby. This leaves enough cords for paramedics and hospital staff to start IV lines.
- Do not tie, clamp, or cut an umbilical cord on a baby who is not breathing unless the cord is around the baby's neck.
12. Re-suction the baby’s mouth and nostrils if the newborn is not breathing or is having respiratory distress.
13. Dry and wrap the baby in a warm blanket and cover its head. One of the greatest risks to a newborn baby is to become hypothermic and hypoglycemic as it attempts to keep warm.
14. Place the newborn on its side to facilitate drainage of nasal and oral secretions.
15. Perform an APGAR assessment at 1 minute and 5 minutes after delivery.
Normal Vitals for Newborns:
- Vital signs:
- Temperature (able to maintain stable body temperature in normal room environment)
- Pulse (normally 120 to 160 beats per minute in the newborn period)
- Breathing rate (normally 40 to 60 breaths per minute in the newborn period)
NOTE:
For premature births, provide the infant with oxygen by blowing oxygen across the infant's face. Insulate the infant to maintain body temperature. Protect the infant from contact or exhaled breath of others who might transmit infections.
APGAR
APGAR Testing and Scoring is assigned in the first few minutes after birth to help identify babies that may need further care. The baby is checked at one minute and five minutes after birth for heart and respiratory rates, muscle tone, reflexes, and color.
Each section/category can have a score of 0, 1, or 2; with 10 points as the maximum. A total score of 10 means a baby is in the best possible condition. Nearly all babies score between eight and 10, with one or two points taken off for blue hands and feet because of immature circulation. If a baby has a difficult time during delivery, this can lower the oxygen levels in the blood, which can lower the Apgar score.
Note: Apgar scores of 3 or less often mean a baby requires immediate interventions such as aggressive stimulation, assisted ventilation, or CPR.
Care of the newborn after delivery:
Once the body has delivered the baby should begin breathing on its own within a few seconds but that may seem like an eternity, be patient, and calm!. If breathing doesn't start spontaneously, you must stimulate it to begin by rubbing the newborn's back or tapping your fingers on the soles of its feet. If the newborn does not start breathing effectively within 10 – 15 seconds of stimulation, use an infant BVM to deliver GENTLE PUFFS of air, just enough to cause the chest to rise. If after 30 seconds of assisted ventilation there is no response and the heart rate is < 60 beats/min, begin CPR, and call for ALS assistance.
Keep the newborn warm by drying it and then wrapping it in warmed blankets. After the umbilical cord is clamped and cut, cover the baby's head to maintain body heat. Be careful because a wet baby is very slippery. Repeat suctioning of the nose and mouth, if needed.
Remember to check the APGAR score at 1 and 5 minutes.
Keep mother and baby safe and warm, place the wrapped baby on the mother's chest for warmth while transporting them to the nearest appropriate facility. Prepare for the delivery of the placenta about 20 minutes after the newborn is delivered.
It is important to realize that the mother may be the more serious patient following a normal delivery. Postpartum hemorrhage can kill. Emphasize that the mother may be a more serious patient.
Postpartum hemorrhage can kill!
Fundal massage over the mother's uterus can help stop postpartum bleeding. It is painful for most mothers to experience directly after childbirth, but nonetheless, it is necessary in the event of excessive hemorrhage. If bleeding is excessive and fundal massage fails to slow or stop the bleeding, request ALS backup so fluids and medications can be administered to help control blood loss.