Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Pediatric Emergencies
Category: Special Populations
Topic: Pediatrics
Level: EMT
Next Unit: Seizures, Adult and Pediatric
15 minute read
Pediatric Emergencies
The most commonly encountered pediatric emergencies are: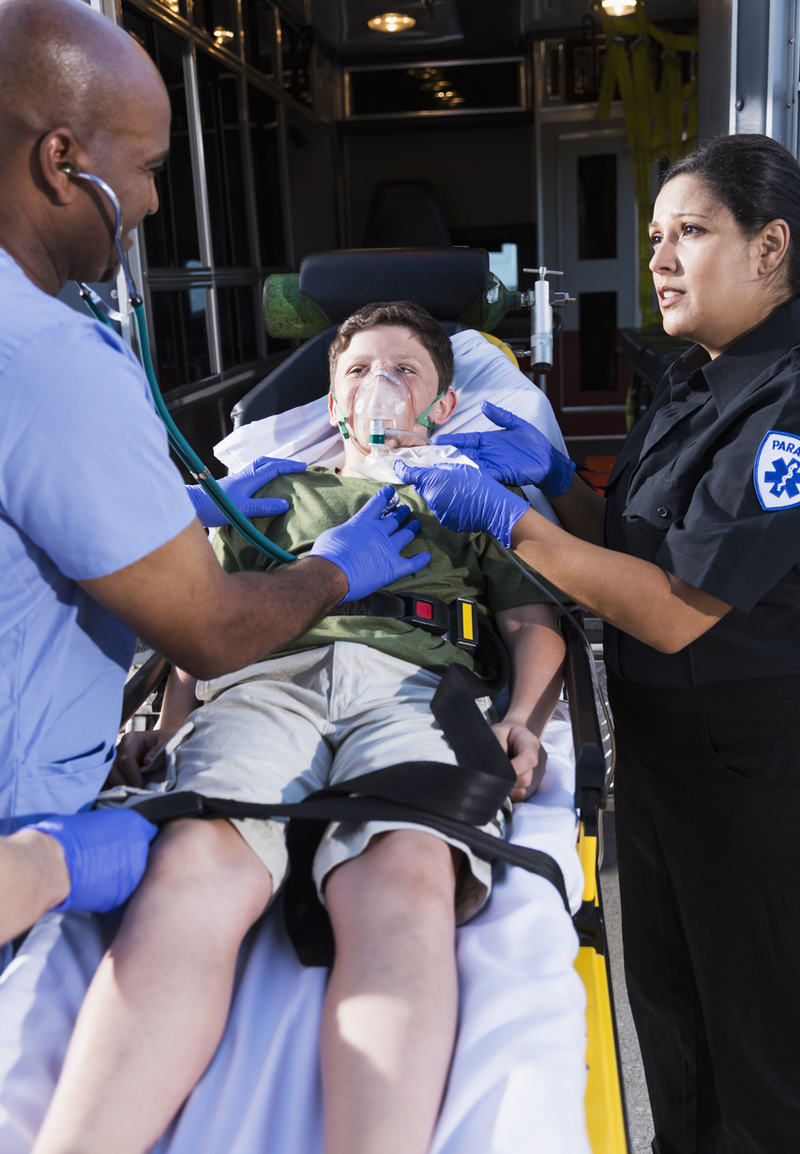
- Respiratory emergencies, including asthma. Status Asthmaticus is an asthma episode not responsive to the usual bronchodilators.
- Neurologic emergency, including seizures.
- Sepsis or severe infection.
- Dehydration: excessive heat loss may occur from the head.
- Anaphylaxis.
- Choking.
- Head trauma--increased in infants and toddlers.
- Cardiopulmonary arrest
Respiratory Emergencies
In respiratory emergencies, use the knowledge you get from your physical findings in conjunction with getting a good history from the patient and his family.
DEFINITIONS:
- Respiratory distress is an increased work of breathing, with tachypnea, use of accessory muscles, and/or retractions. (The "B" of the Pediatric Assessment Triangle.)
- Respiratory failure is the body's inability to circulate enough oxygen to exist.
- Respiratory arrest is the cessation of breathing.
Respiratory complaints account for the majority of cardiopulmonary arrests in children. Therefore, always be vigilant for signs of compensation or shock and be prepared to intervene sharply as kids tend to compensate very well for a period of time, but when they become exhausted, they can crash quickly.
When dealing with respiratory problems in the pediatric patient, it is essential to remember that:
- The overall airway is much smaller than in adults, and the tongue is proportionally larger, causing obstruction more easily.
- Infants younger than 6 months are obligate nose breathers.
- Their tracheal cartilage is softer and more collapsible.
- The epiglottis of infants and toddlers is long, floppy, and extends at a 45-degree angle to the airway.
- The lungs are smaller in kids, and the heart is higher on the child's chest than in adults.
Upper Airway Obstruction
Upper airway obstruction is common in young people and is primarily caused by swelling of the tissue or foreign bodies. (Excessive secretions, such as in asthma, are not upper airway but throughout the bronchopulmonary tree.)
Also, the disproportionate anatomy (as compared to adults) contributes to upper airway obstruction occurring more easily due to:
- prominent occiput (back of the head) influencing neck flexion in the supine position
- large tongue
- larger tonsils and adenoid
- large, floppy epiglottis
- superior laryngeal position causing a more acute angle between the glottis and the tongue
- a shorter, narrower trachea
MANAGEMENT
Managing upper airway obstruction in pediatrics involves correct airway positioning using the chin lift or modified jaw thrust and using finger sweeps, back blows, abdominal thrusts, and suctioning to dislodge the obstruction.
The modification of the jaw thrust that makes it modified is establishing in-line stabilization of the head and neck to move the jaw forward with a minimum head extension.
An oral airway can keep the tongue from obstruction as well.
The patient may require supplemental oxygen or assisted ventilations with a bag valve mask.
Infection
Noteworthy infections that can cause respiratory distress, failure, or arrest are:
- Croup is an infection, usually caused by a virus, in the lower airway.
- Epiglottitis is an infection of the epiglottis, typically with H. flu (Haemophilus influenza), which can cause a child's epiglottis to swell to obstructive proportions and be life-threatening. Routine vaccinations cover this type of infection.
Both croup and epiglottitis can result in sitting upright, drooling, and fever.
Epiglottitis patients can deteriorate VERY RAPIDLY to a complete airway obstruction. Therefore, the conventional wisdom is to use BVM 100% O2 and get to the hospital with frequent reassessment, ready to intubate at any time.
In the Field
In the field:
- Securing the airway may be difficult.
- Opening the airway and obtaining a "sniffing" position may require a towel or roll under the shoulders.
- It is essential to suction the nares of infants in respiratory distress.
- Posterior displacement of the tongue may cause airway obstruction.
- Smaller airways are more easily obstructed by
- Flexion or hyperextension.
- Particulate matter (including mucus).
- Soft tissue swelling (injury, inflammation).
Pediatric Shock
Pediatric shock (hypoperfusion) is the state where the body has insufficiently oxygenated blood getting to tissue.
Children with shock may have normal blood pressures.
Hypotension must be rapidly identified because those with low blood pressures typically deteriorate rapidly to undergo cardiovascular collapse and cardiopulmonary arrest. Measurement with a manual cuff may be more accurate for children with circulatory compromise.
PULSE PRESSURE: When the blood pressure is normal (as can be in compensated shock), shock can be suggested by changes (widening) in the pulse pressure.
PULSE PRESSURE = [SYSTOLIC minus DIASTOLIC numbers]
Narrow pulse pressure: < 30 mmHg when diastolic pressure is increased due to a compensatory increase in systemic vascular resistance (in hypovolemic and cardiogenic shock).
Widening pulse pressure: >40 mmHg reflects diastolic blood pressure decrease as the result of decreased systemic vascular resistance (in distributive shock).
PHYSICAL FINDINGS IN PEDIATRIC SHOCK:
- Elevated heart rate.
- Pale and clammy skin.
- Weak or absent pulse.
- Altered mental status.
When the cause is respiratory, the problem lies in getting oxygen to the blood and should be treated by
- opening the airway,
- correct positioning, and the
- administration of supplemental oxygen or assisted ventilations via bag-valve-mask (BVM).
When there is oxygen getting to the blood but there is insufficient blood volume due to trauma, infections, or excessive fluid loss via vomiting/diarrhea,
- fluid replacement is necessary.
- The total "dose" of IV fluids in a pediatric patient is 20ml/kg
- Hypovolemia from gastroenteritis is the most common cause of shock, followed by trauma and sepsis.
- Temperature: fever is consistent with septic shock, as is purpura.
- Abnormal breath sounds:
- stridor or wheezing: anaphylaxis, as is urticaria or facial edema;
- crackles: pneumonia (septic shock) or heart failure (cardiogenic shock);
- asymmetric breath sounds (tension pneumothorax);
- airway obstruction: may lead to cardiovascular collapse from hypoxemia.