Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Oxygenation, Ventilation, and Respiration
Oxygenation, Ventilation, and Respiration
Cells in our body can only survive in a specific pH range. pH is a measure of how acidic/basic a fluid is. The pH scale ranges from 0 to 14, with 7 being neutral. A pH less than 7 is more acidic, whereas a pH greater than 7 is more basic. The process of oxygenation, ventilation, and respiration are central to maintaining this acid/base balance. Without proper oxygenation, the body will create vast amounts of lactic acid. Without ventilation, oxygenation is impossible, and the body cannot expel carbon dioxide. Without respiration, there is no gas exchange in the lungs or the cells.
This section will focus on the respiratory system's basic physiology and its role in balancing the acid-base status. Critical care transport providers often deal with severely ill patients that are both ventilated and have severe abnormalities in their acid-base status, making this information critical to the care of your patients.
Oxygenation
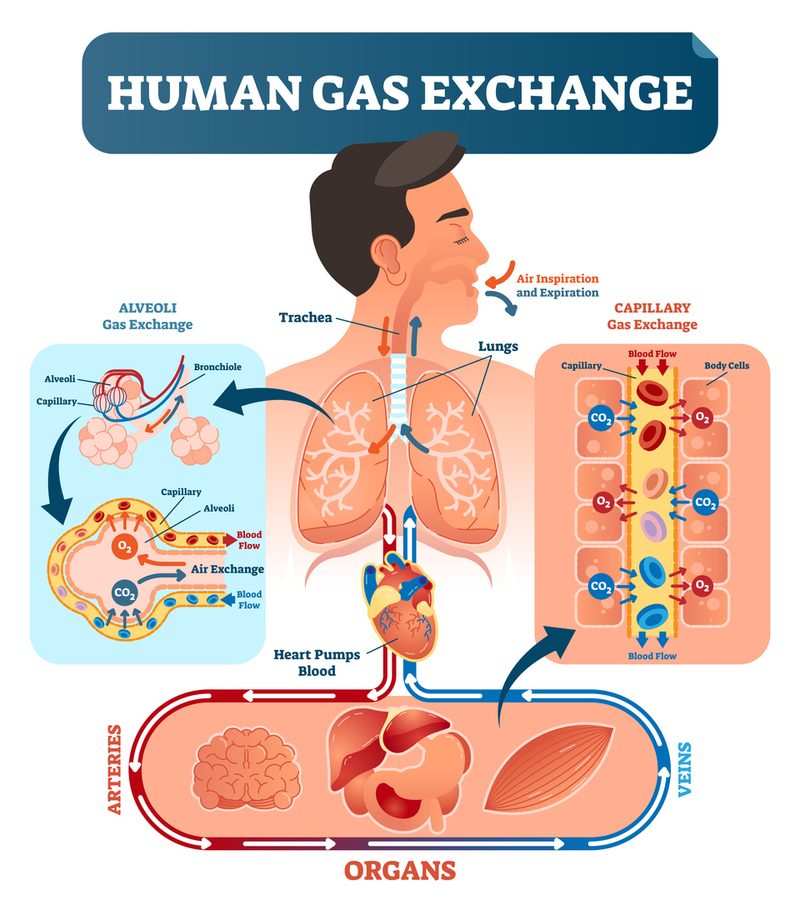
Oxygenation is the process of taking oxygen from the outside air and delivering it to cells. It is a complex process that relies on ventilation, external respiration, internal respiration, and the function of the circulatory system. This section will cover the basic steps of oxygenation and the factors that affect oxygen transport in the blood.
Steps
The main steps required for the oxygenation of cells are as follows:
- Adequate FiO2: The presence of an environment with a sufficient partial pressure of oxygen.
- Ventilation: The ability of the body to move air into and out of the lungs in sufficient volumes.
- External Respiration: The exchange of gases between the air in the alveoli and the lungs capillaries.
- The Presence of Hemoglobin: Oxygen must bind to hemoglobin on red blood cells for transport. 98% of oxygen is transported attached to hemoglobin.
- Adequate Cardiac Output: Blood must be circulating at an adequate rate. This depends primarily on the following three factors.
- Preload: The amount of blood present at the beginning of the heartbeat.
- Contractility: The strength of the heart's contraction.
- Heart rate: The speed at which the heart is beating.
- Perfusion: The presence of capillaries in the tissue being oxygenated and adequate blood flow to those capillaries.
- Internal Respiration: Internal respiration is the transfer of oxygen from the capillaries to the interstitial space and then to the cells.
- Utilization: The ability of the cells to use the oxygen transferred to them in the creation of energy through aerobic respiration.
These same steps reverse to transfer carbon dioxide from the cells into the atmosphere. The only difference is that a larger portion of carbon dioxide travels in the plasma instead of being bound to hemoglobin.
Keep in mind the difference between "internal respiration" and "external respiration." While these processes sound similar, they are very different.
Oxyhemoglobin dissociation curve
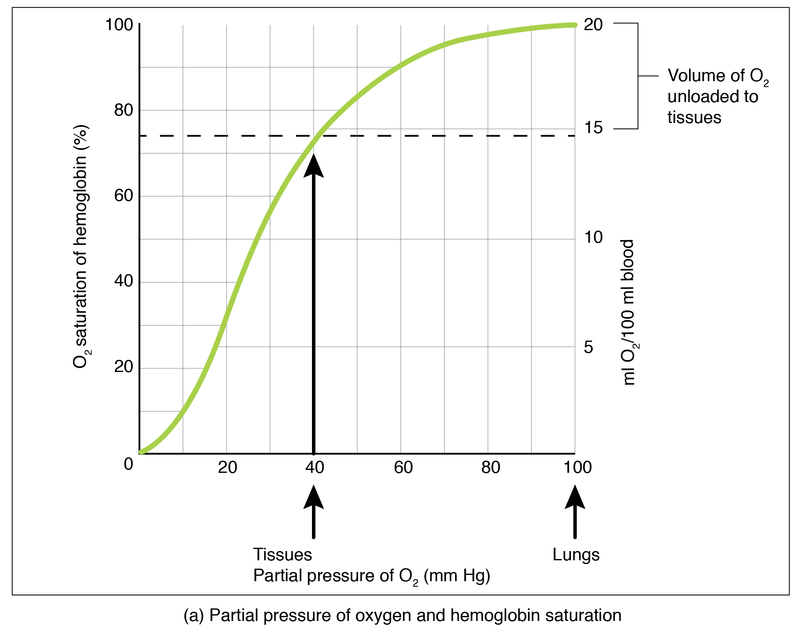
The oxyhemoglobin dissociation curve is a graphical representation of how various factors alter oxygen binding to hemoglobin. If the curve is shifted to the "right," it implies that oxygen is less tightly bound to hemoglobin and more available for cells. If the curve is shifted to the "left," it implies that oxygen binds more tightly to hemoglobin and is less available to cells.
These shifts are relatively unimportant in healthy individuals. Still, in critically ill patients being cared for at altitude, minor changes in the binding of oxygen to hemoglobin can cause hypoxia and acidosis if they go uncorrected.
- Left Shifts: When the curve shifts left, oxygen is bound more tightly.
- Alkalosis
- Low temperature
- 2 - 3 DPG
- Low carbon dioxide levels
- Right Shifts: When the curve shifts right, oxygen is more easily released. A common tool to remember this is that Right shifts are caused by things that start with R.
- Raised levels of acid (acidosis)
- Raised temperature
- Raised levels of 2-3 DPG
- Reduced Oxygen content in the air
A better way to remember these factors is to consider their purpose. Oxygen binding is higher in the lungs to encourage oxygen uptake. It is lower in the capillaries to encourage oxygen release into the cells. In the lungs, there is a lower temperature due to outside air, lower carbon dioxide levels, and a more alkalotic environment due to the aforementioned loss of carbon dioxide. These factors all lead to increased oxygen uptake from the environment to the hemoglobin in the lungs.
Ventilation
Ventilation is the process of physically moving air in and out of the lungs. It relies on a patent airway, the muscles associated with the thoracic cavity, and multiple systems that keep the microscopic air passages in the lungs clear of debris and obstructions.
Inspiration
Inspiration, moving air into the lungs from the environment, is an active process. It requires the use of muscles, specifically the diaphragm, intercostals, trapezius, and neck muscles. These muscles expand the chest cavity, lowering the pressure within the chest and pulling air into the lungs through the trachea like a vacuum.
- Inhalation requires
- Adequate muscle strength
- A patent airway
- The ability of the chest wall to expand
- Inhalation is compromised by:
- Loss of muscle strength
- Loss of airway patency
- Damage to the chest wall that prevents negative pressure within the chest cavity from forming.
- Nearly any issue with inhalation can be solved with intubation and positive pressure ventilation.
Exhalation
Exhalation, the process of moving air out of the lungs to the environment, is a passive process. The natural elastic recoil of the lung tissue pulls the tissue together after the muscles used for inhalation are relaxed. The intercostals in the chest wall also assist with this process as they help pull the ribs closer together.
- Exhalation requires:
- Adequate elastic tissue in the lungs
- A patent airway
- Exhalation is compromised by:
- Loss of elastic tissue (as seen with COPD and emphysema)
- Increased airway resistance due to blockage of small airways
- Loss of airway patency
- Unlike inhalation, intubation and positive pressure ventilation will not always solve exhalation issues. Intubated patients can still have severe issues with air trapping and delayed exhalation that leads to acidosis through hypoxia and carbon dioxide buildup. Agents to open small airways such as beta-agonists and anticholinergics can help with exhalation.
- If you are using a full ventilator as opposed to a transport ventilator, altering the inspiratory and expiratory times will help with exhalation.
- Choosing a longer expiratory time, 3x to 4x the inspiratory time may be necessary in the setting of severe asthma or COPD.
- This is an advanced intervention that will vary based on your local protocols and specific equipment.
Respiration
Respiration (external respiration) is the process of exchanging oxygen between the blood and the various environments inside and outside of the body. Respiration (internal respiration) also involves utilizing oxygen in the body to create energy.
External Respiration
External respiration is the goal of ventilation. Oxygen present in the alveoli diffuses into the oxygen-poor blood in the lungs, and carbon dioxide from this same blood diffuses into the alveoli. This exchange relies on sufficient blood flow, alveolar surface area, and the presence of a large volume of air.
- External respiration relies on
- A large number of intact and ventilated alveoli.
- Capillaries close to the alveolar walls that have blood flowing through them.
- External respiration is compromised by
- Destruction of the alveoli leads to decreased surface area for diffusion (as seen in COPD).
- Blockage of alveoli (as seen in pneumonia, ARDS, and drowning).
- Reduced blood flow to the lungs (as seen in shock and pulmonary embolism).
- External respiration will improve with PEEP. This forces open more alveoli, increasing the surface area for respiration and increasing the oxygen diffusion rate.
Internal Respiration
Internal respiration is the process of oxygen diffusing from the capillaries into the body's various cells. This process is driven by the massive amount of oxygen attached to hemoglobin and the relatively low oxygen levels in the fluid surrounding the cells. Internal respiration also refers to the process of creating energy from oxygen and disposing of waste products from said process. This information is complex but vital to your understanding of acid-base balance in the setting of shock.
- Internal respiration relies on
- Adequate flow of oxygenated blood to cells
- The diffusion of oxygen from the capillaries, to the interstitial space, into cells, and then into the mitochondria (which are the powerhouses of the cell).
- The presence of glucose or fatty acids.
- Internal respiration can be inhibited by
- The absence of oxygen
- The absence of glucose, insulin, or fatty acids from fat breakdown.
- The presence of toxins that prevent mitochondria from functioning (cyanide and aspirin overdose are classic examples).
The process of creating energy from oxygen is known as aerobic respiration and occurs as follows:
- Glucose is split into Pyruvic acid
- Pyruvate enters the Krebs cycle and generates electron-rich byproducts
- The electron-rich byproducts are converted into large amounts of ATP (energy) in the mitochondria
- Waste carbon dioxide diffuses out of the cell
Creating energy without oxygen is known as anaerobic respiration and occurs as follows:
- Glucose is split into pyruvic acid
- The absence of oxygen drives the body to convert pyruvate into lactic acid for the creation of ATP as opposed to into the Krebs cycle.
- The waste lactic acid is ejected into the bloodstream.