Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Basics and Management of Soft Tissue Injuries
Category: Trauma
Topic: Soft Tissue Trauma
Level: EMT
Next Unit: Pathophysiology of Wound Healing
33 minute read
Soft Tissue Injury Basics
Superficial skin injuries are some of the most commonly encountered injuries. While rarely dangerous on their own, they are commonly present in patients with more severe underlying conditions. The ones to know are:
- Abrasions
- Lacerations
- Punctures
- Bites
ABRASIONS: superficial wounds where the outermost layer of skin is scraped or rubbed off.
- "Road Rash" from a fall is a common abrasion.
- These injuries can be extremely painful as they involve the layer of the skin that contains the nerves.
- These injuries rarely bleed excessively once they have been dressed or had pressure applied to them for a short time.
LACERATIONS: a cut in the skin caused by impact with a sharp object. (A micro-assessment of lacerations shows that all are, in fact, tears--when a pressure exerted against the skin creates a force beyond which the skin's normal elasticity can tolerate.)
- The edges are usually rough or jagged unless the object was extremely sharp.
- Depending on the severity of the laceration, bleeding may be minimal or severe depending on the depth of the cut and involvement of deeper and larger blood vessels.
PUNCTURES: different than lacerations because the force is directed towards the body, as opposed to across the body in a laceration. (Like lacerations, technically punctures are tears.)
- Puncture wounds leave a wound in the shape of the offending object.
- All punctures must be assessed for the presence of an exit wound which is created when the penetrating object traverses the body completely and leaves a second wound with a tract connecting them.
- Removing the clothing and assessing all skin surfaces is vital and a key step in assessing these patients.
- Impaled Objects: These are penetrating objects that are stuck through the skin. As per other chapters, penetrating objects should not be removed. Applying a bulky dressing and stabilizing the object for transport is key.
BITES: Bites from insects or animals are another type of open soft trauma injury.
- Human bites are considered an emergency as they can become seriously infected.
- Transport is appropriate for a serious human bite.
- Animal bites are of varying concern.
- Bites from insects and some reptiles can be poisonous.
- Bites from large animals can obviously be severely traumatic, and smaller mammals may be hosts for various diseases, such as rabies.
Eye Injuries
Eye injuries are a unique category of soft tissue injury. Even simple things such as grit, metal dust, or chemicals that are harmless to skin can cause severe injury to the eye.
- Redness, tears, pain, and blurring of vision are key signs of eye injuries.
Management
Treatment of abrasions, lacerations, punctures, and bites is focused around the use of dressings--sterile pieces of cloth that absorb blood and help compress the wound and control bleeding. They come in many shapes and sizes. Bandages go over dressings and hold them in place.
For eye injuries, pre-hospital procedures for dealing with foreign bodies or abrasions to the eye are
- to lay the patient flat and tilt their head to the affected side, so that whatever is in it does not get into the unaffected eye.
- Hold the patient's eyelid open with one hand, using the orbital bones for gentle leverage. Never press onto the eye itself.
- Flush the affected eye for at least 15 minutes with water or normal saline.
(For alkali burns--more damaging to the eyes than acids--even more flushing is necessary.)
Soft Tissue Injuries

There are countless possible forms that soft tissue injuries can take. Regardless of the severity, these injuries are managed in the same way, with external compression and pressure.
Soft tissue injuries take many forms. Those that bleed externally are universally managed with compression and pressure dressings. All external dressings are a variation on this theme, the remainder of this section will discuss the differences between these modalities.
STERILE GAUZE: The simple placement of sterile gauze over a wound and applying pressure with a gloved hand is the go-to traumatic dressing for a wide variety of situations. Everything from scrapes to stab wounds can be served by this dressing. Never remove gauze that is soaked with blood, as this may disrupt a forming clot! More severe bleeding or patients that require the rescuer to use both hands for other interventions may require one of the more advanced interventions listed below.
SECURED GAUZE: This intervention replaces the source of compression, switching from the rescuer's hand to tape and a specialized pressure bandage. This can increase the pressure on the wound compared to a hand and allows the rescuer to attend to other injuries or interventions.
MECHANICAL SPLINTING: Certain wounds on extremities are amenable to the placement of rigid support over the gauze that is covering the wound. This offers support to any damaged bones, compression over a wide area, and can act as a partial tourniquet, further slowing the rate of bleeding.
PNEUMATIC TOURNIQUET: Often the simple inflation of a blood pressure cuff upstream of the injured blood vessels on a limb, the pneumatic tourniquet is a quickly adjustable method of cutting off the blood flow to an area. Often used for any form of arterial bleeding, tourniquets can reduce the internal bleeding that occurs with arterial injury to a limb. Whenever applying a tourniquet, it is important to note the time of application, as this has implications for the patient's treatment later in the emergency room.
MECHANICAL TOURNIQUET: Using the same philosophy as a pneumatic tourniquet, the mechanical version is generally used for more severe bleeds. There are several types of mechanical devices and you should be familiar with the version that your jurisdiction requires you to carry. Mechanical tourniquets generally cause more trauma to tissue than pneumatic variants but are less prone to failure when used correctly.
COMPLICATIONS OF TOURNIQUETS: Placing a tourniquet (of any type) can result in temporary or permanent nerve damage in a matter of minutes, limiting their use to situations where direct compression has failed. Even if nerve damage is temporary, placement for over 2 hours often results in ischemic damage to the limb, with times over 6 hours generally requiring partial or complete amputation. EVEN SO, the use of a tourniquet SAVES LIVES.
Management of Bleeding Patients
Keep bleeding patients calm, warm, and lying flat to prevent falls from sudden lightheadedness and further shock from hypothermia. Ensure that you complete the remainder of your assessment after you have stopped the bleeding, as secondary injuries may be present.
The prehospital management of bleeding at the EMR level revolves around holding pressure on the site to slow loss of blood and arranging rapid transport. At the EMT/Paramedic level, administration of intravenous saline and/or blood, products are routinely warranted.
Note that there are different types of bleeding, capillary bleeding causes a slowly oozing wound, venous bleeding presents with dark flowing non-pulsatile bleeding, and arterial bleeding is bright red and is pulsatile, often spurting with severe injuries.
REASSESSMENT: Bleeding patients should be assessed for the development of blood loss symptoms often. Exactly how often depends on the severity of the bleeding. A patient with a minor capillary bleed will likely be fine all throughout transport. While a patient with a major arterial bleed may require interventions on a minute-by-minute basis to keep them alive.
Some of the symptoms that signify a transition from mild blood loss to clinically significant blood loss are: weakening pulses in the extremities, fatigue, somnolence, pale/cold/clammy skin, increasing tachycardia, shortness of breath at rest, and changing mental status (confusion, aggression, inappropriate laughter).
These symptoms should be noted and recorded for a patient with known or suspected blood loss.
Management of Soft Tissue Injuries
Soft tissue injuries can be divided into two rough categories, open and closed. This division is based on whether the skin is broken or not.
Both types of injury have the potential to be life-threatening, but open injuries require additional pre-hospital care to minimize potential morbidity and mortality. This section will examine open and closed injuries separately, along with treatment considerations for each.
Presentation of Closed Soft Tissue Injury
Closed soft tissue injuries are injuries to an area of the body where the skin is left intact. The 3 major types are contusions, hematomas, and crush injuries.
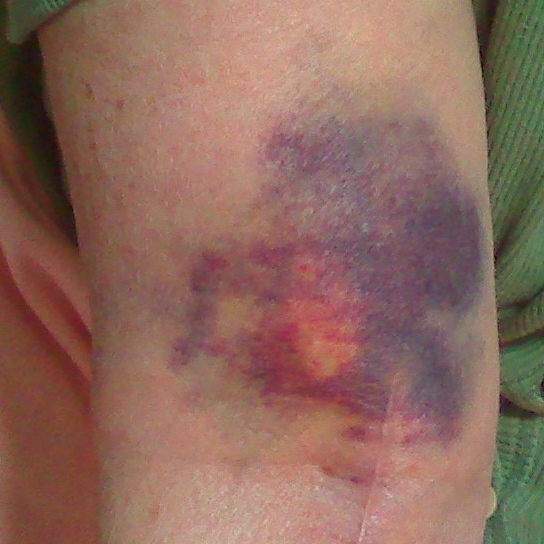
CONTUSIONS are bruises. They occur when the tissue of the skin or beneath the skin has taken blunt force, damaging the small blood vessels.
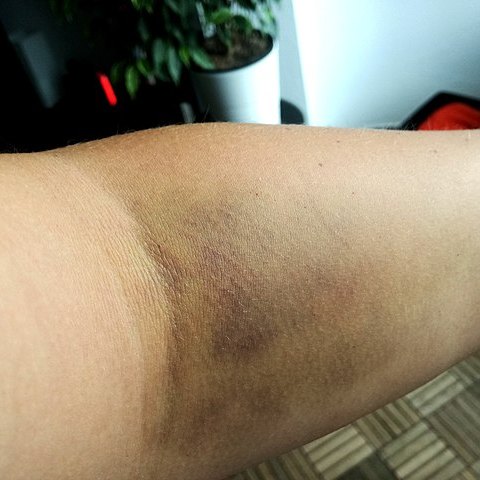
HEMATOMAS are large bruises with an underlying collection of blood that forms a lump beneath the skin, tending to form when larger blood vessels are damaged.
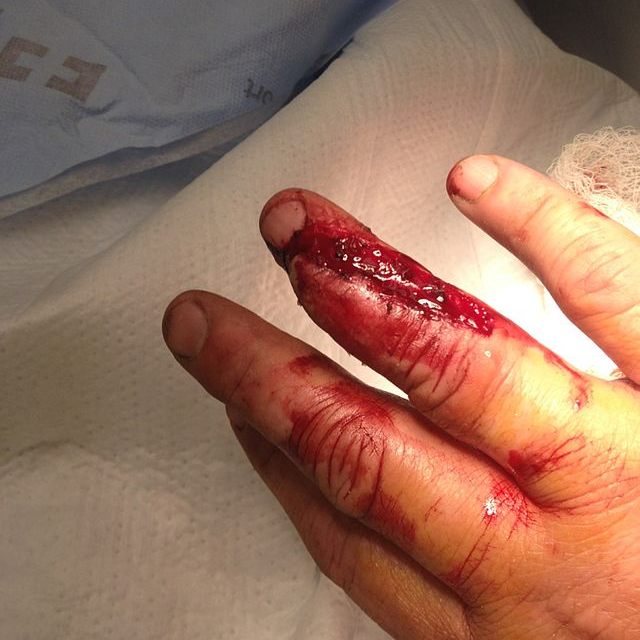
CRUSH INJURIES result from the traumatic compression of tissue, usually against an underlying bone.
Closed soft tissue injuries present with pain, swelling, and discoloration of the overlying skin. They may be a sign of deeper internal injury, so you should have a high index of suspicion for underlying injury in patients with significant closed soft tissue injuries.
MANAGEMENT OF CLOSED SOFT TISSUE INJURY
When managing closed soft tissue injuries, rule out damage to underlying neurovascular structures by ensuring distal PMS in all affected limbs (pulse, motor function, and sensation.)
Management of these injuries is focused around R.I.C.E.S--an extension of the classic acronym RICE (rest, ice, compression, elevation). Injuries to the trunk, neck, and head should be managed similarly, with a focus on ice and direct pressure and regular reassessment of the ABC's to watch for internal injury.
I.C.E.S.
- Ice - to constrict blood vessels, reducing swelling and numbing pain.
- Compression - reduces hematoma formation and can also assist with swelling.
- Elevation - again, reduces blood pooling and swelling.
- Splinting (the added item in the acronym) - can assist in providing compression to the injury and preventing further injury from movement.
ABCs: In closed tissue injury to the face, head, or neck, increased swelling may result in airway compromise. If the patient begins to become unstable, always shift your focus to maintaining an open and secure airway, adequate breathing, and adequate tissue perfusion.
Presentation of Open Soft Tissue Injury
Common open soft tissue injuries include abrasions, lacerations, puncture wounds, bites, avulsions, and amputations.
Each of these injuries come in a wide variety of severities, but regardless of the severity, there are two major concerns in all open soft tissue injuries, hemorrhage and infection.
HEMORRHAGE: loss of blood becomes a concern when enough is lost that shock develops and perfusion to tissues is lost.
Penetrating trauma, deep lacerations, and amputations are especially likely to lead to hemorrhagic shock.
Abrasions, avulsions, and minor lacerations can lead to shock if left unmanaged or in patients with conditions that predispose them to bleeding.
INFECTION: a risk with any injury that penetrates the skin, the main barrier which keeps bacteria and other potentially harmful microorganisms out of the body.
Infection can lead to loss of life or limb late in the course of an injury.
As with most medical conditions, prevention is the most effective treatment, and therefore this is the reason EMS professionals are often the first to sterilize and dress a wound.
MANAGEMENT OF OPEN SOFT TISSUE INJURY
Open injuries are similar to closed injuries in that damage to underlying structures is a constant concern. Even superficial injuries can overlie significant internal trauma, so evaluating the patient's ABC's and distal PMS in limbs is of significant importance.
Open injuries require management of bleeding and protection from infection, the steps of which are outlined below:
- Ensure BSI (body substance isolation).
- Ensure an open airway, adequate ventilation, and tissue perfusion (circulation).
- Apply an occlusive dressing to open chest injuries.
- Apply direct pressure over any open wound with a dry, sterile dressing.
- Apply pressure dressing or compressive splint
- If bleeding continues or recurs, apply a tourniquet to an extremity above the level of bleeding.
- Be alert for and treat for shock (hypoperfusion) by raising legs, fluid administration, maintaining body temperature, and administering high-concentration oxygen where appropriate.
CAVEATS:
- Whenever applying pressure dressings or splinting, always check to make sure distal pulses remain palpable.
- Never remove a flap of skin regardless of size as complete avulsions dramatically increase the risk of infection compared to those with a skin flap in place.
- Wash the wound with sterile saline, then return the skin to a normal anatomical position if possible. Then proceed to the steps outlined above for dressing the wound.
- Do not remove any impaled objects unless they compromise the airway or impede chest compressions.
NOTE: As with closed injury, If there is damage to the airway, face, or neck, increased bleeding into or around the airway will compromise the airway. If the patient begins to become unstable, always shift your focus to maintaining an open and secure airway, adequate breathing, and adequate tissue perfusion (ABC).
