Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Basics of Orthopedic Trauma
Category: Trauma
Topic: Orthopedic Trauma
Level: EMT
Next Unit: Splints and Immobilization
14 minute read
Fractures
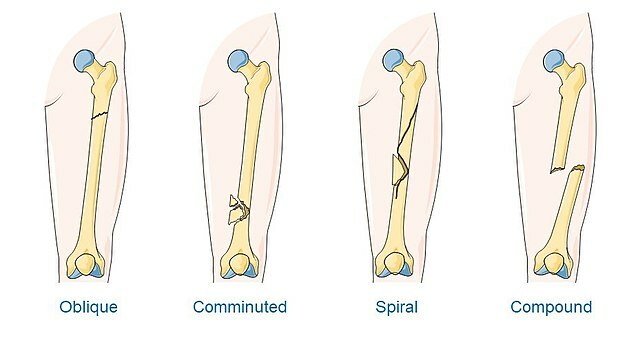
The most common fractures occur in the extremities and collarbone. In general, a bone fracture is not usually a life-threatening injury, but any fracture can be dangerous if it is able to do damage to the vessels and organs around it. So, while a toe fracture is not likely to become emergent, pelvic and femur fractures have a high risk of resulting in serious blood loss.
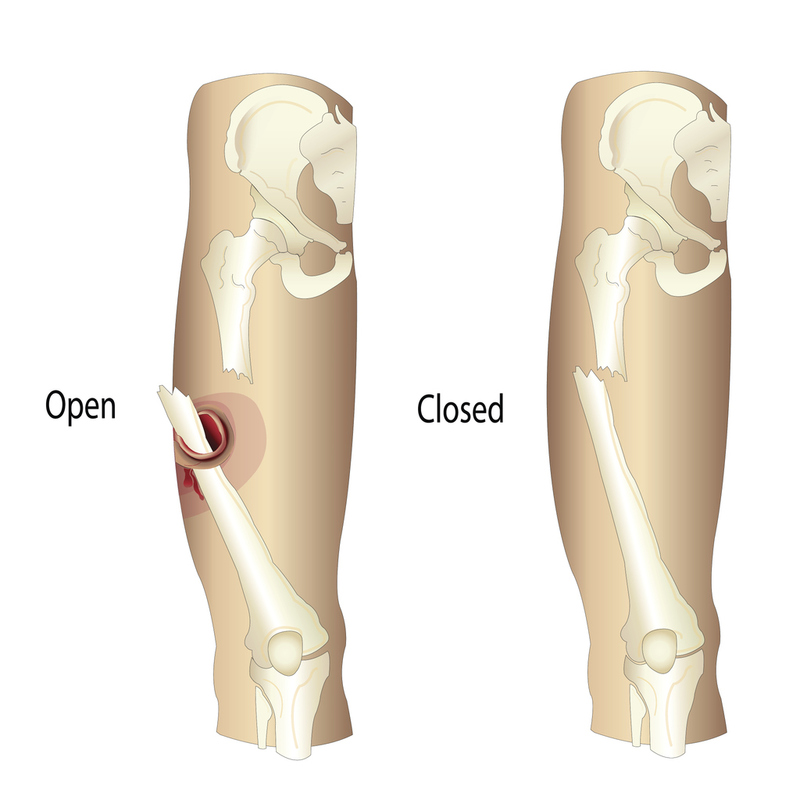
- OPEN FRACTURE: any bone fracture that results in the bone piercing through the skin or being exposed to the environment outside the body. (The term, "compound fracture," is an open fracture, although "open fracture" is preferred due to the other term making it sound like fractures in multiple locations.)
- CLOSED FRACTURE: a bone fracture that does not result in the broken bone breaching the protection of the skin.
As with any trauma that breaks or damages the skin, cover any open wounds with a sterile dressing. This is of particular concern in fractures given the high risk of osteomyelitis, or "bone infection," in patients with open fractures.
Fractures create sharp edges and mobile pieces of bone, both large and small, inside the body; these pieces or shards can sever nerves and vessels or injure tissues around the bone. This secondary mechanism of injury can occur long after the initial trauma.
MANAGEMENT: In many cases, manual stabilization may be required to limit further damage.
- When possible, allow the patient to be in a position of comfort.
- Secure the long bone or joint above and below the injury site so as to restrict movement of the damaged limb without putting direct pressure on the injury site.
- Cover any open wounds with a sterile dressing, pad any air spaces that allow for motion of the limb, and apply cold packs to the affected area to reduce swelling and pain.
Do not intentionally manipulate any exposed bones into going back below the skin, because broken bone fragments can do further damage to tissue and vessels around the injury site. Surgery is required for proper closure in all cases of open fracture.
Dislocations
Dislocations occur when the bones themselves are not broken but become dislodged from their proper position at a joint. Dislocations can be hard to distinguish from fractures, as they may both be extremely painful, swollen, and disabling. In a dislocation, deformity or angulation at the location of a joint is often apparent. The bones, while dislocated, can rub together and cause grating or limitation of motion. Other signs and symptoms of dislocation include distal pulselessness, paresthesia, or paralysis due to neurovascular compression at the site of the dislocation.
The most common sites for dislocation are the acromioclavicular joint which connects the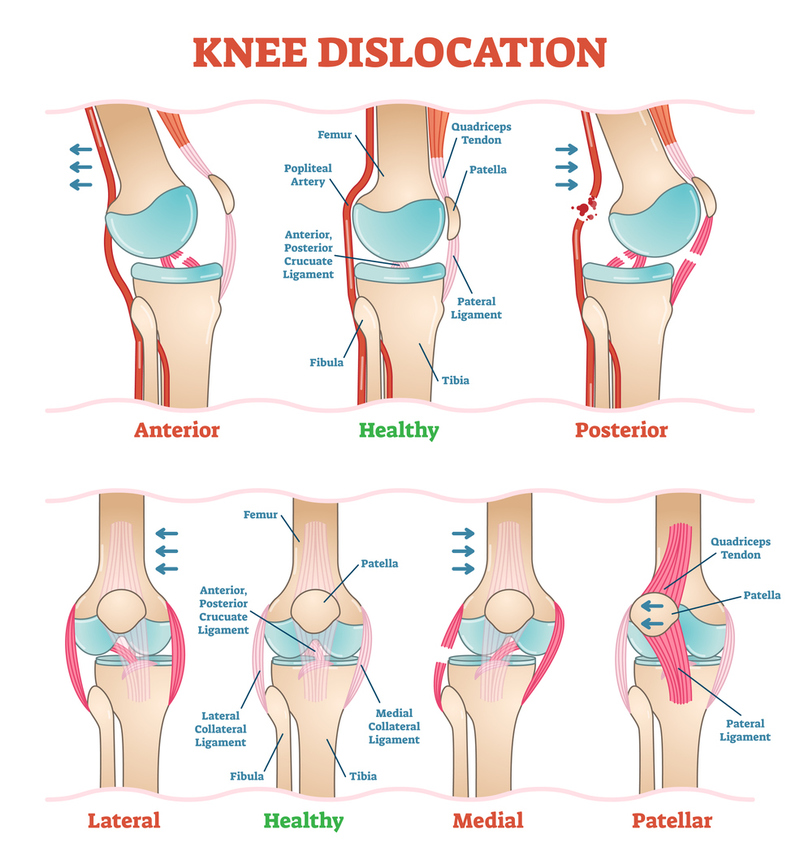 collarbone to the shoulder, the shoulder itself, the elbow, wrists, and fingers. The hip and knee can also become dislocated. Hip fractures may also cause the hip joint to be unstable and cause the femur to slip out of the socket.
collarbone to the shoulder, the shoulder itself, the elbow, wrists, and fingers. The hip and knee can also become dislocated. Hip fractures may also cause the hip joint to be unstable and cause the femur to slip out of the socket.
Distinguishing between dislocations and fractures can be difficult. The telltale sign of dislocation would be an obvious deformity, but both share pain, swelling, and bruising. Dislocations can have the effect of locking the joint since the disarticulated portion of the joint is no longer seated in its socket.
There are joints at many locations in the human body which are not entirely obvious. Some of the oft-forgotten are those of the anterior shoulder, namely the acromioclavicular and sternoclavicular joints.
MANAGEMENT:
- After life threats have been controlled, apply a cold pack to the deformed area to reduce swelling and pain.
- Extremity stabilization may be required to prevent movement, just as in fracture.
- Make sure to stabilize the injury ABOVE and BELOW the injury site, putting as little pressure as possible on the affected area.
- Cover any open wounds with sterile dressings.
Amputations
An amputation is when a limb or part of a limb has been cut from the body. As a general rule, the more proximal the amputation, the greater the threat to life and the greater the level of care required.
For example, with amputations of a finger, bleeding is much easier to control than when an entire leg is amputated.
MANAGEMENT:
- Elevate the injury
- Apply ice to help slow blood flow.
- Cover the location of the missing body part with a dry, sterile dressing.
- Apply direct pressure (Plan A for hemostasis.)
- Once bleeding is controlled, immobilize the area to prevent further damage to microscopic structures and the disruption of fragile clots.
- If you cannot control bleeding in the stump with direct pressure alone, the use of a tourniquet may become necessary. (Plan B for hemostasis.)

Place these devices as close to the injury as possible while avoiding joints. 1" wide straps are sufficient for the upper limbs 1.5" is the minimum for the lower limbs. Write the time of application on the strap when placing it.
- If you have access to the severed body part, place it in a sealed plastic bag and put that bag in a bowl of ice water and send it to the hospital with the patient.
- Do not put the amputated body part directly onto the ice and do not let the amputated part become saturated with water. All amputated body parts should be saved even if they appear unsalvageable as the part may become valuable material for plastic surgeons to reconstruct other damaged parts of the patient's body.