Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Asystole and PEA
Category: Cardiology
Topic: Advanced Cardiac Life Support
Level: Paramedic
Next Unit: ACLS Tachycardia
11 minute read
Asystole and PEA
You arrive at the scene of an unconscious patient. He is unresponsive, does not show evidence of breathing, and has no palpable pulse. If there is no pulse, the heart is not functioning, and we need to start it again. In this unit, we will explore these life-threatening situations and the algorithmic approach to tackling them.
Recognition of Asystole and PEA
ASYSTOLE means "no contractions" in the heart, but the full definition means no mechanical or electrical activity in the heart. Asystole refers to the complete cessation of electrical activity in the heart, signified by a "flatline" on the ECG, no palpable pulse, and no heart sounds. This condition is not shockable and requires immediate initiation of high-quality CPR and advanced interventions. EMS providers should confirm asystole in two different leads and rule out the possibility of a loose lead or technical issue causing the flat line.
PEA stands for "Pulseless Electrical Activity," meaning there is still electrical activity in the heart. Still, it is not coordinated in a way that allows the heart to function correctly to produce a pulse, even if there are contractions. (A "shimmying" heart.) The presence of an organized ECG rhythm without a palpable pulse also indicates PEA. EMS providers should assess the patient's pulse and breathing and evaluate the ECG rhythm for potential underlying causes. This condition is not shockable and requires immediate initiation of high-quality CPR and advanced interventions.
Management of Asystole and PEA
When the heart isn't contracting properly, oxygenated blood is not moving around the body. Providing high-quality CPR is the best initial way to ensure blood will circulate.
Excellent CPR and early defibrillation for treatable arrhythmias remain the standards 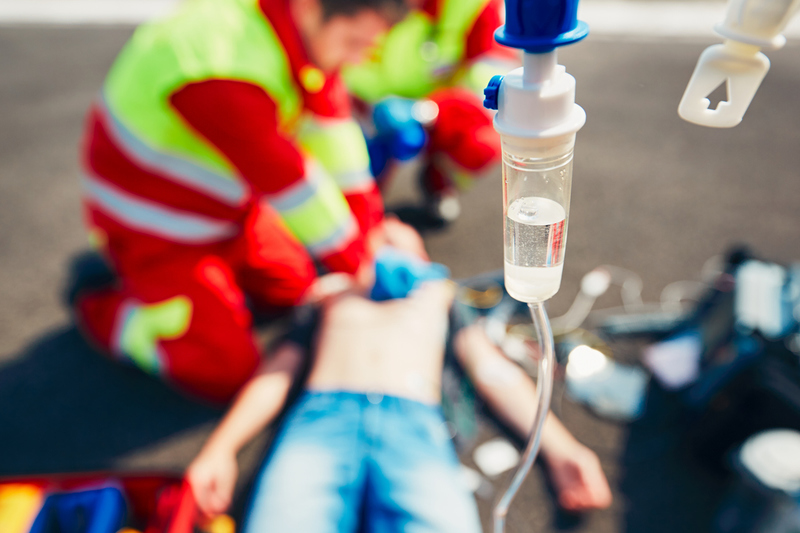 for basic and advanced cardiac life support:
for basic and advanced cardiac life support:
- Perform high-quality CPR. EMS providers must ensure proper chest compression depth, a rate of 100-120 per minute, full recoil of the chest after compression, and minimize interruptions as much as possible.
- Secure and maintain an adequate airway and provide adequate ventilation with supplemental oxygen.
- Monitor the victim's heart rhythm and blood pressure to keep apprised of changes.
►Asystole and PEA are NOT shockable rhythms. - Continue high-quality CPR cycles while attempting to establish IV or IO access until the rhythm changes.
- After an IV/IO access has been established, give 1mg of Epinephrine 1:10,000 IV as soon as possible and every 3-5 minutes during CPR to improve coronary perfusion and increase the chances of return of spontaneous circulation (ROSC).
Ruling Out Reversible Causes
Always consider and treat any potentially reversible causes of asystole or PEA. If your patient is in aystole due to a problem that we can solve, we fix that underlying problem and restore circulation. Remember the H's and T's as possible triggers: Hypoxia (lack of oxygen), Hypovolemia (not enough fluid in the body), Hypothermia (Freezing), Hyper/hypokalemia (Too much or too little potassium), Hydrogen ion (acidosis), Tension pneumothorax, Tamponade (cardiac), Toxins (ingestion or overdose), and Thrombosis (pulmonary and coronary clots).
ROSC
If the patient attains Return of Spontaneous Circulation (ROSC), provide Post Cardiac Arrest Care.
After ROSC, the full AHA algorithm includes the following:
Respiratory care to optimize ventilation and oxygenation.
A > 94% SAT is optimal.
IV/IO access, if it hadn't been established already.
Cardiovascular care, including interventions, hemodynamic goals, and vasopressors.
Treat hypotension with 1-2 L normal saline/LR-epinephrine (vasopressor) infusion.
Amiodarone can treat most atrial arrhythmias (recurrence after ROSC) but is used primarily to maintain normal sinus rhythm in patients with atrial fibrillation (AF).
Treat reversible causes of the arrest, if applicable (Hs and Ts).
ASSESS: Can the patient follow commands?
If so, run a 12-lead EKG to determine if there is STEMI.
If not, other critical care interventions, such as glucose control and targeted temperature management (TTM), previously called "induced therapeutic hypothermia," may be indicated according to your local medical director's established protocols. The decision to implement TTM (32-36 ° C, 89.6-96.8 ° F) is based on whether a patient can follow commands: reserved for unresponsive patients to prevent neurological injury.